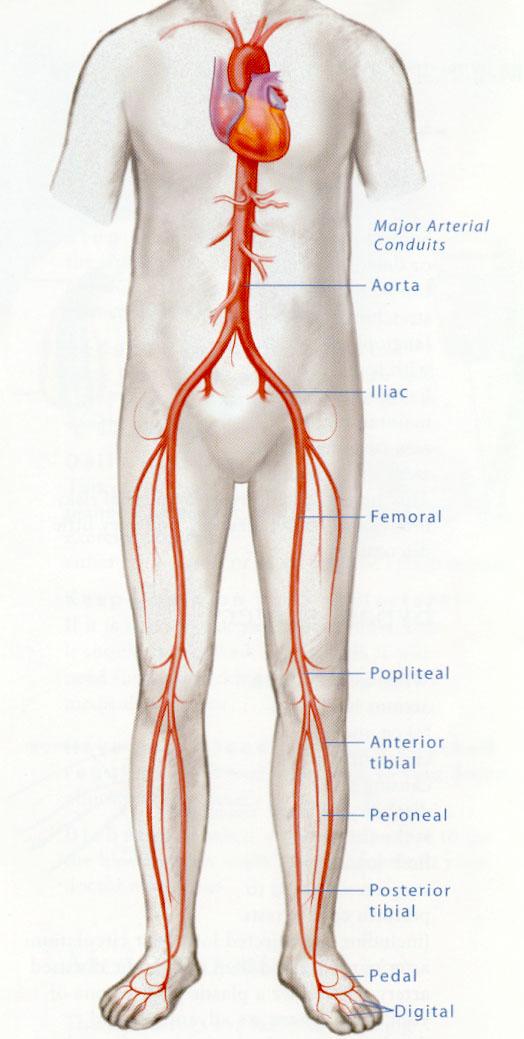

Peripheral Arterial Disease Peripheral arterial disease (PAD) is most commonly caused by atherosclerosis or hardening of the arteries. This common affliction can go unnoticed for many years because it usually progresses slowly and onset of symptoms is gradual until it is finally diagnosed. The presence of arterial insufficiency produces very specific symptoms and therefore diagnosis can often be made by a careful history and physical examination. Simply feeling for pulses can alert the physician to the presence of any significant artery blockages. Very often testing may be indicated to determine the severity and pattern of the disease and establish unequivocally if the symptoms you experience are due to PAD. Testing can be done non-invasively and consists of a variety of techniques that can measure the pressure and volume of blood in the affected limb. If this is abnormal, a complete overview of the circulation in the legs is most often made with ultrasound, a relatively inexpensive, completely safe and noninvasive technique that obtains pictures of the vessels and information about the blood flow in real time. No other technique provides both the anatomic and physiologic information which is of prime importance in PAD. How the lower extremity artery system works - The arterial system is a series of branching vessels all originating from the heart—the central pump of the body. Similar to tree branches, the arteries become smaller and smaller as they extend to the periphery of the body. the aorta is the main artery that arises from the heart and gives rise to all other arteries. The abdominial aorta branches into the iliac arteries at the umbilicus or belly button. These in turn branch again and again until vessels course all the away to the abdomen.
ATHEROSCLEROSIS - Normally the inner wall of an artery called the intima is smooth and elastic, allowing blood to flow freely. In vessels affected by atherosclerosis, the intima becomes thickened and rough by a build up cholesterol or fatty materials. This build up, much like rust in a pipe, is called plaque. As this plaque increases, it obstructs the opening or lumen of the blood vessel and may alter or limit the flow of blood. If the artery is severely narrowed, the amount of blood getting past can be so limited, that various symptoms can result. However, as long as this is a gradual process, the body is often very good at developing alternative pathways for blood flow called collaterals. SYMPTOMS -
There are other reasons why a person may experience leg pain with exertion or even at rest - commonly neuropathy or a nerve compression (neurospinal) syndrome. The testing equipment at QVI is well suited to determine with a high degree of certainty if pain is from a vascular cause (vasculogenic) or not. DIAGNOSIS - is typically done with a combination of physiologic testing and duplex ultrasound (click for more on these testing procedures.) This non-invasive test can determine if disease is present, its severity, and if it is a likely source of your symptoms. We can also provide an overview of the arterial tree showing the pattern of disease. For example, it is important to know specifically where the disease is, if there is an isolated area of narrowing or is there diffuse disease throughout long segments, and if a vessel is severely narrowed of completely occluded. This information allows your physician to make specific recommendations as to the best way to treat your disease.
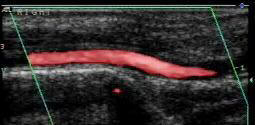
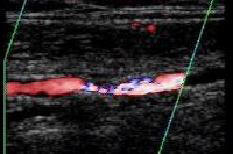
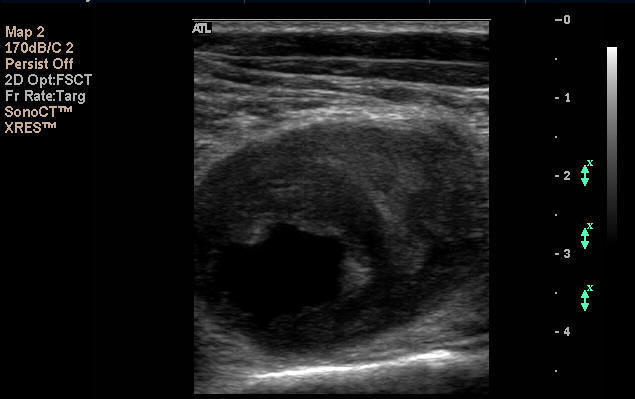
These ultrasound images show tibial arteries in the calf. The vessel on the left depicted in gray scale with the Doppler information displayed in color is widely patent and normal. In contrast, the vessel on the right shows a severe narrowing with the resultant flow disturbance.
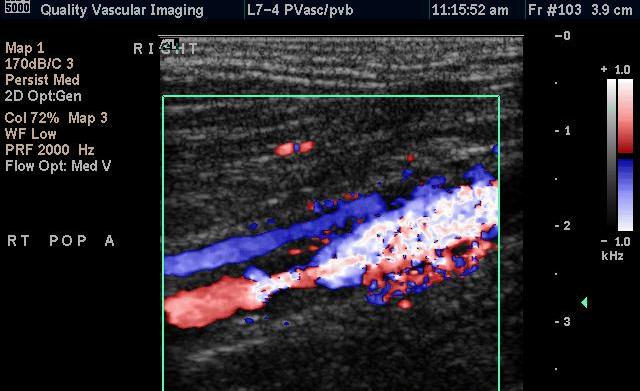
The vessel on the left shows a flow limiting narrowing in the popliteal artery behind the knee - the main blood supply to the lower leg. The popliteal artery on the right reveals a large aneurysm with thrombus inside. While peripheral artery aneuryms rarely rupture, they are potentially quite dangerous if they shower this thrombus to the lower leg. TREATMENT -
Here is a great link from the Society of Vascular Surgery that thoroughly outlines the all the options - Society of Vascular Surgery |
QVI Home Virtual Vein Center Why QVI really is the Best in Vascular Ultrasound! Case of the Month Patients Referring Physicians Health Professionals Site Map |
Current Happenings

Introducing our new educational website.

Virtual Vein Center is a new concept in educational delivery. Get the education you need and want, when you need it. If you need CME, you can get them here as well.
To read more about it, click here for a complete page. Feel free to go to the site and browse around.


Several QVI staff took time to attend the 2014 American College of Phlebology Annual Congress in Phoenix Arizona in November to deliver numerous workshops and lectures. It was a high quality meeting as usual. The complete program is available for download here.


The 2014 SVU Annual Conference was held in Orlando and several QVI attended and presented numerous presentations. Jeannie was also honored as a Fellow of the SVU.
To read more

Jeannie recently attended the 25th Society of Vascular Medicine 2014 Annual Conference as an invited speaker in La Jolla, Ca. Her numerous lectures were very well received.


The International Union of Phlebology, in conjunction with the American College of Phlebology held its World Meeting in Boston in September 2013. Held only every 4 years, this was the first time ever in the US. Several QVI staff were invited speakers presenting some original scientific research.

Sydney, Australia

Bill was the International Keynote Speaker at the Australian Sonographer Association Annual National Conference in Sydney.
What a great experience!
To read more about this and our other international teaching


QVI was once again awarded the D.E. Strandness Award for Scientific Excellence at the 2013 SVU Annual Conference.
To read more -

Medical Compression socks continue to be on the forefront of venous treatment. Recently, they have entered the realm of the athlete. To learn more about what compression socks can do you you, please visit compressionsocks.pro


QVI wins the D.E Strandness Award at the 2012 SVU Annual Conference!
Read more about it!

To go to the
CASE OF THE MONTH!
Click the QVI logo